If you want to prevent cancer, cut sugar! This is the message of an Oct. 13, 2017 study. The research team had done experiments for 9 years, when they concluded that it was refined sugar that caused spontaneous mutations of RAS proteins. RAS proteins are responsible for cell growth. When a substance like sugar turns them on all the time, they can cause mutations that lead to cancer. In this article research concentrated on yeast cells, and the publication is in Nature Publication. The CNN publication describes this in simpler language. Essentially the research team found that a sugar molecule, fructose-1,6-bisphosphate, was responsible in obese patients and in diabetic patients to mutate a RAS protein, which as a result can turn into an oncogene causing cancer.
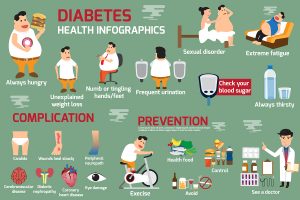
Evidence that sugar causes obesity and type 2 diabetes
- A September 2017 US study followed 41 children age 9 to 18 with initial fructose consumption of >50 g/d. The treatment of the children consisted of an isocaloric fructose restriction of only 9 days. Following that their liver fat content decreased from 7.2% to 3.8%. In addition intraabdominal fat decreased and new fat production was reduced from 68% to 26%. The authors pointed out that reduction of sugar consumption in obese children was a very effective treatment tool.
- This August 2017 study from Helsinki followed 71 obese males for 12 weeks. They consumed 75 grams of added fructose every day in addition to their normal food intake. The liver fat content increased and cardiovascular risk factors worsened as blood tests showed. The investigators concluded that the adverse cardiometabolic effects were a result of the added fructose. They were not secondary to the weight gain (a theory in the past).
- This February 2017 study from the US the Taiwanese Healthy Aging Longitudinal Study in Taiwan was also of interest. It consisted of a 5-year long study involving middle-aged and elderly patients with type 2 diabetes. The result was that patients with more physical activity, a better diet and a higher score regarding psychosocial health did much better with respect to managing their diabetes. Maintaining a healthy lifestyle is particularly important for the elderly to prevent diabetes.
Evidence that obese patients and type 2 diabetics get more cancer
- In this 2016 study from Poland the effect of diabetes causing various cancers was under investigation. The authors pointed out that worldwide in 2014 there were 387 million cases of type 2 diabetes and it was still rising. When they looked at correlation between various cancers and type 2 diabetes they found that diabetes had the strongest association between pancreatic cancer and liver cancer. But there was also an association between diabetes and breast cancer, bladder cancer and kidney cancer. Head and neck cancers were more frequent among diabetics. Some diabetic medications made cancer frequencies worse, others, like metformin made them better.
- In this March 2016 article from the BJC (British Journal of Cancer) cancer frequencies were correlated to patients with obesity and to patients with diabetes. Researchers found that some types of cancer correlated with obesity, whereas others did with diabetes and not with obesity. They found that type 1 diabetes had its own set of cancer risks while type 2 diabetes had a different set of cancers that correlated to the disease
More on cancer risks in diabetics
- A 2015 study from Malaysia with an 11-year follow-up describes that type 2 diabetes had increased in the population which researchers studied. The investigators concentrated on a female population where they found a strong correlation between diabetes and endometrial cancer, ovarian cancer, breast cancer and cervical cancer. In a group of 860 cancer patients they found that 26.5% were diabetics. They were at a much higher risk of getting these cancers.
- A 2016 study from the US examined 2,836 veterans who had problems with their esophagus. 1,704 received a diagnosis of esophageal adenocarcinoma, 1,132 of them had gastroesophageal reflux disorder. Among the cancer patients there were 30.8% diabetics. The researchers calculated that for diabetics there was a 2.2-fold higher risk of developing esophageal cancer. The only other risk factor they could identify was nicotine dependence, which showed an association with a 1.7-fold risk of to develop esophageal cancer.
Evidence that sugar causes cancer
As explained earlier research found that fructose-1,6-bisphosphate is responsible in yeast cells to lead to RAS mutations. Human cells have the same metabolism as yeast cells, and they also have RAS protein and fructose-1,6-bisphosphate. Fructose-1,6-bisphosphate is important for cancer development in humans. Yeast cells are diploid cells as are human cells. But yeast cells are not human organisms, so the parallel stops at one point.
- A 2014 study from China showed that fructose-bisphosphate aldolase was a marker for lung cancer metastases. This enzyme breaks down fructose-1,6-bisphosphate. Depletion of fructose-bisphosphate aldolase A reduces cell motility of cancer cells and the ability to cause more tumors. In other words, the key for cancer cells to thrive is the presence of fructose-1,6-bisphosphate.
- In this 2013 study from Beijing gastric cancer biopsies research examined these samples for fructose-1,6-bisphosphatase, the enzyme that breaks down fructose-1,6-bisphosphate.
The enzyme was under expressed in 86.2% of the gastric cancer biopsies. This meant that glycolysis was stimulated in the cancer cells. An overabundance of fructose-1,6-bisphosphate caused tumor cells to get into an active phase and to metastasize.
Discussion of why sugar causes cancer
I have previously discussed this topic in a blog 3 ½ years ago. At the time a few steps were missing from the knowledge we have today. Nothing has become different regarding the connection of sugar overconsumption and the risk of developing cancer. First of all, we have learnt that fructose overconsumption or sugar overconsumption leads to fructose-1,6-bisphosphate in the blood, which stimulates RAS proteins to mutate and stimulate oncogenes to cause cancer. In addition, people who are overweight, obese or have diabetes have too much insulin production, which can also lead to cancer causation. Finally, obese people have a lot of very active kinins in the blood that can cause cancer as well. In conclusion, what has changed between March 2014 and now is that we have a lot more detail why things happen the way they do. Connections that used to be obscure have now a rational explanation.
The message is that we need to cut out refined sugar from our diet, cut out starchy foods and cut out processed foods. This will improve our metabolism and reduce our risk of getting cancer. We will also lose weight, which I have experienced in 2011 when I lost 50 pounds over 3 months. What did I do? I was just doing what I described to you: cutting out sugar, starchy foods and processed foods.
Conclusion
Want to reduce your risk for getting cancer drastically? Then cut out sugar and starchy foods along with processed foods (which have too much sugar in it). Strangely enough it was only now that researchers have found the missing link. The culprit is fructose-1,6-bisphosphate, a metabolic byproduct from sugar consumption. It stimulates a RAS gene, which can mutate, turn into an oncogene and eventually cause cancer. This fact was not known a few years ago. But the knowledge that cancer can occur due to diabetes, obesity and insulin resistance goes back a long time.
We need to learn from science: cut out refined sugar, starchy foods and processed foods. This will change insulin resistance into insulin sensitivity. Fructose-1,6-bisphosphate will not accumulate, but get normally metabolized. This way fructose-1,6-bisphosphate does not pose a problem for RAS proteins. Your insulin level will normalize, the previous kinin overproduction will disappear and your risk for cancer will decrease.
We have allowed the sugar industry to undermine our health for too long. It is time to take back the control over our lives, assess our food habits and make the necessary changes.