Recently I traveled from Palm Springs to the Caribbean and back and I had to think: what a wonderful world! There were connecting flights and there was waiting at various airports. I had lots of time to watch people and to observe what was happening around me. Louis Armstrong’s song (1967) “What a Wonderful World“ came to mind. I thought that this would be a fitting title for this Blog. Earlier we had come from Canada escaping the winter. The deep blue sky of Southern California and the sight of palm trees (instead of pine trees) is something that makes our hearts beat faster.
The desert is a special place
The desert is a special place. We had friends join us for a week and we had visited Joshua Tree Park with the grotesque looking rock formations. During the flight it was interesting to see the landscape, as we crossed the desert areas of Arizona and New Mexico, seeing what difference people make when large areas are irrigated and the desert transforms into lush, green areas. It is also very visible, where the desert has taken back the land that no longer is irrigated.
Travel to Dallas Fort Worth and Miami
We came to Dallas Fort Worth and the sky was clear. We traveled on to Miami and the sky was showing signs of pollution, although it was a sunny day. After our take-off from Miami we saw the ocean. I have flown over that region many times before, but this time I detected oil slicks on the surface of the ocean of the Gulf of Mexico, leftovers from previous oil spills. So, the Armstrong song of a “wonderful world” came back to me in a different context. I looked at the landscape and what industries can do to it. Erroneously we had just seen several BP commercials while waiting for our plane at the airport where BP was congratulating itself for the role it plays in cleaning up the environment having spent several billion dollars. But there are still oil slicks…
Watching people on the plane
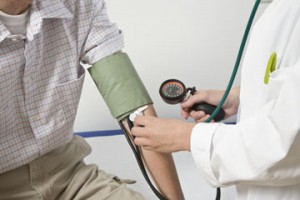
I looked at the people around me in the plane. More than 35% of them were obese; many of their faces looked sagging and prematurely aged, particularly in women. Males, even middle aged ones looked like they were pregnant (abdominal fat) and often their hair was receding, thinning on top and quite a few were bald. All of the texts I had read about anti-aging medicine came back to me. Too bad that people were eating the wrong foods and obviously did nothing to counter their built-in aging clock from depleting hormones as we age.
Menu of the airline
I looked at the menu of the airline. I won’t mention the name of the airline, but I can assure you that 10 different airlines would have almost the same menus. There would only have been one chicken salad that I could have eaten. In the past I tried to order this and I was told that due to popular demand this item was sold out. Instead they wanted to offer me potato chips, cheese and crackers. My wife and I had anticipated this scenario and we had bought a chicken salad and water before we boarded the plane. We also had packed healthy organic energy bars and a trail mix consisting of nuts and raisins to use as snacks during the trip.
Cutting out starchy foods, eating fresh vegetables and lean meat instead
While travelling we stuck to the same principal of cutting out starches, bread, rice, pasta and only eating fresh vegetables, salads and lean meat (chicken, grass fed beef, ribs, lean pork and veal), which we always do since the fall of 2001. We also avoid all alcoholic beverages and sugar containing sodas. When we returned to Southern California we were delighted to see that our body compositions when measured with the body composition scales were identical to what they were before the trip.
I think we can all contribute to this wonderful world, if we participate in whatever we can do such as these steps.
End wars
End wars because on the long-term they do not lead anywhere to solve conflicts (in my lifetime I am thinking about the Vietnam war, long-winded Ireland crisis, the Korean war and the German reunification at the end of the Cold War). Right now there is the Middle East conflict, which screams for a peaceful solution. As we are conscious about the devastation that is caused by wars, we have to start with ourselves. We have to resolve our own conflicts that may be present in our own lives. Tolerance, acceptance and forgiveness are the tools.
Address pollution
Pollution needs to be addressed by the US and all of the world’s countries (including Canada where I live most of the time). This means that anti-pollution devices need to be installed in industrial plants and chimneys. Recycling needs to be done on a larger scale. China and India and other emerging market countries need to be taught how these new anti-pollution measures work. This is an ongoing project, but we need more co-operations between government, industry and countries all around the globe. Also we have to start with our own behavior: we can become more aware of reusing and recycling instead of creating more waste in our landfills.
Become better caretakers of our bodies
What can we do to make us part of this wonderful world? We need to become better caretakers of our bodies. Instead of looking at quantity we must look at quality in choosing natural food wherever possible. Growing up in Germany after the Second World War in the 1960’s and early 1970’s made me witness that high consumption of fat, sugar and starchy foods (potatoes, pasta and bread) caused people to age prematurely and get heart attacks, strokes, high blood pressure, arthritis, obesity, diabetes and cancer. At that time the “Wirtschaftswunder” (translated into English it means “economic miracle”) had propelled Germany into a nation of high consumers. During the war they had been poor and often went hungry, they were slim and heart attacks were at an all-time low.
Unhealthy foods and snacks
After the war they made up for times of deprivation and overindulged: pretzels, buns, bread, butter, French fries, sweets, cakes, cookies, jams, chocolates, pralines-everything was consumed with gusto! What happened to Germany in the 1960’s and 1970’s is happening again right now in front of our eyes with the obesity wave in the US, Canada and all the other civilized countries around the world. Food companies have been very successful with their advertising through the media. Already kids get hooked to the wrong foods! Hyperinsulinism will ensure that we get hungry every two or three hours. Refined carbs and extra calories are turned into fatty acids by the liver and stored as fat. It shows that we have to resist the wrong food temptation and cut out all refined carbs.
Healthier alternatives
It is healthier to stick to salads and vegetables like broccoli, cauliflower, asparagus, and spinach and eat a small piece of lean meat with it. Have probiotics as plain yoghurt (0% to 2% fat). If you need a sweetener, use a small amount of Stevia, which is a natural sweetener that leaves your body chemistry untouched. Have some fruit as a dessert like blueberries, cherries or strawberries. Eat an apple, the occasional grape. Drink lots of purified water or mineral water.
Buy organic food
Buy ORGANIC food whenever possible. Farmers treat most of the vegetables and fruit with insecticides, which contain residuals in them. When these are ingested, they act like estrogenic substances causing breast cancer in women and prostate cancer in men. The safest in our society is to stick to organic foods. More expensive, but the best insurance against future disease. Question politicians whenever possible to make yourself heard. You want unadulterated food and water. And as I’m writing about water, have a water filter under the kitchen sink with a carbon filter. In addition, it is good to have reverse osmosis to get rid of chloride or fluoride from the city water. This is what you use to cook your food. You may want to take an iodine tablet once or twice a day to counteract the negative effects of chlorine from having a bath or shower (the skin absorbs chlorine). Why? Because chlorine and fluoride can displace the iodine of the thyroid hormones and make you hypothyroid.
Regular exercise
Exercise every day. Nobody gets fit in their muscles from sitting in front of the TV for hours. You also don’t get fit from spending hours and hours of computer work. If you have to, counterbalance this with an exercise program of 1 hour per day. Walk 30 minutes on a treadmill and do 30 minutes of weights or use specific exercise machines in a gym to strengthen your upper and lower extremity muscles.
Replace missing hormones with bioidentical ones
Did I mention hormones? Yes, I did above when I mentioned depleting hormones as we age. We know for some time that each hormone of the body has its own peak in life and then it declines in production as we age. Or should I rather say, we age when these hormones decline? I like the latter way of wording it, because we can measure hormone levels and when one of the hormones is too low, we can replace it with a bio-identical hormone and the person’s energy comes back and whatever function was missing is restored. This is in essence what anti-aging medicine does. Many conservative physicians and clinics do not like to hear this. Big Pharma does not like to hear this when I am talking about replacing hormones in the body with bio-identical hormones. But the patented cheap copies that are mass manufactured and sold at inflated prices are no fit to the hormone receptors in the body and therefore are dangerous. The artificial drugs cause heart attacks, strokes and cancer as the Women’s Health Initiative has shown in 2002.
What people need to do
What did I think the people I watched on the plane should have done? Their physicians should have tested the hormones of many of them. Many of the overweight or obese patients would likely have had high fasting insulin levels. The extra fat does not just sit there; it is a hormone producing factory for inflammatory compounds and estrogen-like substances. This causes heart attacks and strokes in women. It causes prostate cancer and hair loss in males as well as impotence (“erectile dysfunction”). What I said above would help these people that I met. When you lose fat through changes in the diet and when you start an exercise program, the body mass index slowly comes down as fat melts away. The estrogen production comes down, the inflammatory substances abate. The person feels more energetic and may even think straighter. This is when you realize what a wonderful world it is.
Saliva hormone test
One special test is a saliva hormone test that looks at 5 steroid hormones: DHEA-S (storage form of DHEA), testosterone, estradiol, progesterone and cortisol. Every man and every woman needs a certain balance between these hormones and this test should be done when there is a change in energy or appearance (hair loss) somewhere when we are 35 to 40 years. In women it is important that the progesterone level is 200 times fold higher than the estradiol level (progesterone/estradiol ratio) or she is at risk of developing breast cancer and other cancers (ovary, colon etc.). In a man it is important that his testosterone to estradiol ratio is higher than 20 to 1. This protects him from cancer of the prostate or other cancers.
Bioidentical hormone creams
The physician or a knowledgeable naturopath can prescribe whatever hormones are missing. The health care provider needs to be familiar with the use of bio-identical hormone creams. This program can prevent diseases like osteoporosis, diabetes, cancer and arthritis. It also prevents disabilities.
With this I leave 2012 behind and I am looking forward to a new year (2013). I am looking forward to the time when more people can see Louis Armstrong’s vision of a “What a wonderful world”.
More information on:
1. Pollution: https://www.askdrray.com/protecting-yourself-from-environmental-toxins/
2. Obesity: https://www.askdrray.com/stop-obesity/
3. Processed food: https://www.askdrray.com/caution-processed-food-ahead/