General practitioners see a lot of patients with various pain symptoms for which they seek pain treatment. The underlying conditions might be from an arthritic problem that suddenly becomes symptomatic, or an acute back injury may send pain from the lower back into one of the legs. Others may experience excruciating headaches like migraines or tension type headaches. Often these painful conditions require some immediate pain relievers to treat the pain, but this can turn into a nightmare of drug dependency and may even lead to the development of chronic pain. Here I like to review an article that I found in the June edition of ConsumersReports.org. In my review I included most of the content, but added a few newer pain treatment modalities.
Acute pain
Here I’m discussing back pain as an example. When a disc bursts in the lower back because the person was lifting an object too heavy to lift, acute pain develops in the lower back. This is often located at the lower lumbar spine level (L5/S1) causing radiating pain into one of the legs.
In a case like this it will often take several weeks before the body can heal this condition.
Chronic pain
It can happen in many cases that the pain will still be there 3 to 6 months down the road. If a disc fragment pushes on the nerve root in the nearby canal through which the nerve root travels, this will cause the muscles supplied by the nerve root to melt away in the leg of the affected side. If nothing is done about this, the acute pain turns into chronic pain, which is much more difficult to resolve. The initial physician may refer the patient to a neurosurgeon who will review the case together with the help of an MRI scan that shows the underlying pathology. The neurosurgeon may determine that a mini discectomy will reduce the pressure onto the nerve root.
Relief of pressure on nerve root from mini discectomy
This surgery may be able to prevent chronic pain from setting in. Once the pressure is relieved, the nerve can start the healing process. It is critical to not miss the point where acute pain crosses over into chronic pain. This happens at around 2 to 3 months into the pain condition. Chronic pain is much more difficult to treat as some of the neurological pain pathways that form after such injuries can persist within the spinal cord or even within the central nervous system, even after successful disc surgery that is done too late. With respect to the example given above, if the patient is operated on too late (1 to 2 years after the injury), the procedure may not be effective in relieving the pain. A chronic pain syndrome has started.
How pain treatment is done
-
Avoid bed rest
In the past (up to the late 1970’s to mid 1980’s bed rest was the accepted initial mode of treatment. Even though patients often felt some relief of pain initially, this led to muscle atrophy (literally a melting away of muscles) in the muscles that are supporting the spine. These structural changes destabilized the spine and often made the pain more chronic until physiotherapy treatments and active exercises rebuilt the supporting muscles again.
-
See a physiotherapist
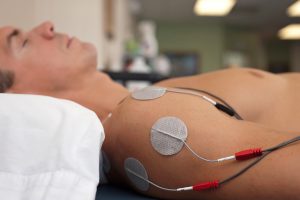
Physiotherapists can use different treatment modalities like traction, a TENS machine, active exercises that all can help to alleviate back pain due to muscle spasm. If there is only a strain, this will often help to resolve your back pain within 4 weeks. But if there is an underlying disc herniation as previously explained, you need to be assessed by a physician in an urgent care center, primary care setting or by an emergency physician in the emergency department of a hospital. When the examination confirms an abnormal reflex from a nerve root compression, a referral to a neurosurgeon or orthopedic surgeon is usually made as previously explained.
-
Chiropractic treatment
Some people have their backs treated periodically to prevent back troubles. When they get an acute back pain they likely will see the chiropractor again. In cases of a back strain, where one or more muscles are pulled, this approach will be helpful together with some home exercises and swimming to build up muscle strength along the spine. However, in the case of a herniated disc chiropractic adjustments should not be done (physicians say they are “contra-indicated”). Instead the patient should be referred to either a neurosurgeon or an orthopedic surgeon.
-
Medication for pain
Often physicians prescribe Tylenol with codeine, hydrocodone (Vicodin), oxycodone (OxyContin, Percocet) or morphine for pain relief. All narcotic medication have side-effects; they can cause constipation, can cause vomiting, make you feel dizzy and can lead to falls, particularly in elderly patients. These falls can cause hip fractures and other fractures that complicate the recovery from the original pain. Never exceed the dosage of pain medicine prescribed on the label, and if it does not relieve the pain, see your physician again for a reassessment to rule out any complications.
Depression with back pain
Often people with back pain also have depression. To address this issue your physician may prescribe an antidepressant like duloxetine (Cymbalta), which has been approved by the FDA for treatment of lower back pain. But there are two rare, but important side effects to know about. Cymbalta can cause lowering of blood pressure, which leads to dizziness. This can cause serious falls with the danger of fractures. The other complication is the risk of liver failure.
Side effects of pain treatment
Pain pills can be addicting
While there seems to be an urgency to treat a patient who is in pain with pain medication, the treating physician must not forget that pain medication is potentially addicting and patients often use higher doses than advisable. However, pain medication has a narrow therapeutic window meaning that the toxic levels are not much higher than the drug levels necessary to relieve pain.
Some medications are only marginally effective
There are medications that are only marginally effective, if at all. Glucosamine and chondroitin are used for relief of arthritic pain in osteoarthritis sufferers. They are eliminated by a liver enzyme system that also eliminates blood thinners. If a patient is on blood thinners, the addition of glucosamine and chondroitin can lead to dangerous bleeding. Instead of using glucosamine and chondroitin when you experience pain and inflammation in joints, reduce your activities, but stay as active as you can to avoid your symptoms from getting worse.
Tests for severe migraines
When a patient has a severe migraine headache it is tempting to want to rule out a brain tumor. But a CT scan exposes the patient to dangerously high radiation doses that over time could cause brain cancer or leukemia. There are physical examination methods to rule out a brain tumor. If the findings are positive, an MRI scan can be used to get much more detail of the brain than a CT study would reveal. MRI scans do not have undesirable side effects.
Use gentle movement to remobilize the painful joints
Before you rush into using anti-inflammatory drugs, use gentle movement to remobilize the painful joint, back or limb. Activities like swimming, walking or yoga can reduce pain and allow you to recover from a painful condition according to a Cochrane Library analysis of 61 studies.
Non steroidal anti inflammatory drugs (NSADs)
For more pain relief NSAID (non steroidal anti inflammatory drugs) pain relievers like ibuprofen (Advil) or naproxen (Aleve) for a brief period will also help. The problem with long-term use of NSAIDs is that it can cause kidney damage. With longer use of NSAIDs there is also a danger of stomach bleeding, heart attacks and strokes.
Toxicity with Tylenol
The pain drug acetaminophen (Tylenol) has a narrow therapeutic window and is less effective in pain relief than the NSAIDs. The FDA has recommended as the highest daily dose 4000 mg of acetaminophen. But if you are a heavy drinker or you have liver disease, your daily dose of acetaminophen should not exceed 3250 mg to avoid liver toxicity. Long-term use of acetaminophen can also damage your kidneys, therefore the recommendation to use acetaminophen only for a short period of time (a few days).
Side effects of triptan drugs for migraines
Migraine headache drugs: The newer migraine drugs, called triptans temporarily narrow widened blood vessels. This relieves severe migraines within about 2 hours. However, these medications are not recommended for those with high blood pressure, chest pain, heart disease or circulation problems in the legs, as blood vessel constriction could bring on heart attacks or worsen circulation problems.
Common sense approach to pain treatment
The key for any pain condition is to treat the pain right away to minimize the impact that pain has on you and to prevent developing chronic pain, which is more difficult to treat.
Here are some examples.
Migraine headaches
If you have a migraine headache, use an over-the-counter pain reliever like naproxen or ibuprofen to treat the migraine pain very early. A combination of acetaminophen, aspirin and caffeine (like Excedrin Migraine or a generic copy) will also do. This will stop the release of prostaglandins, which would send pain signals to the brain. Heat packs or cold packs on your head can also help in the treatment of a headache. A 2013 study from Germany has shown that migraine sufferers can get rid of their migraine headaches in 60% by having sex. It sounds like a nice idea, but what they have not considered may be the fact that somebody who has a splitting headache is not feeling like sex at all!
Triptan pills for migraines
If your home remedies did not help, see your physician for one of the triptan pills. Sumatriptan or a similar drug constricts blood vessels to the brain. The doctor will also look for common triggering factors that can bring on a migraine. Weak neck and shoulder muscles may respond to physiotherapy strengthening. In women a condition called estrogen dominance is associated with migraines and can be treated with bioidentical progesterone to balance estrogen and progesterone in the body by elevating progesterone concentration.
Acute lower back pain
Acute lower back pain usually follows an event where the person lifted something too heavy or injured the back from a fall. The important part is to rule out a fracture. Most of the time there is no underlying fracture, just a muscle strain. A muscle strain usually sorts itself out in time. Stay active as much as possible. But if the back pain does not resolve within a few days, see your physician for more tests. X-rays can delineate structural changes like a fracture. As explained earlier, an MRI scan can rule out a disc herniation. Instead of neurosurgery, further options nowadays are prolotherapy, stem cell therapy or a combination prolotherapy/stem cell therapy. This type of therapy will also work for knee injuries (meniscal or ligamentous tears).
Hip or knee pain
Conventional medicine usually treats osteoarthritis with NSAIDs, but may not warn you about the possibility of gastric erosions that can lead to massive stomach bleeding, heart attacks or strokes when using NSAIDs. It also can lead to kidney damage that can cause sudden kidney failure. The key is to use anti-inflammatory medication only for a few weeks. If arthritis persists, it is wiser to seek the advice of a naturopathic physician for prolotherapy treatment. One or two treatments of prolotherapy can give relief of pain. If prolotherapy does not succeed, it is best to move on to mixed stem cell therapy with bone marrow and mesenchymal stem cells (from fat cells) as well as PRP (platelet rich plasma). This usually leads to complete healing of osteoarthritis and eliminates the need of total knee or total hip replacement.
Neck and shoulder pain
This often develops because of poor posture, shoulder tendinitis or neck muscle spasm. Physiotherapy is often successful treating this. If not the physiotherapist can use intramuscular stimulation (IMS) with acupuncture needles. This may be more successful in interrupting the abnormal neuropathic pain pathways. Alternatively electro acupuncture with a TENS-like device can also be successful. The newest treatment modality is the Weber medical system using a low-dose laser applicator. Prolotherapy can also be used for shoulder and neck problems, if the ligaments are lax. It requires a lot of experience on behalf of the health professional to choose the right treatment protocol for the condition.
Tension headaches
Anxiety, stress and fatigue can all lead to tension headaches. Initially you may want to drink liquids, as dehydration is related to tension headaches. If your headache is still present after one hour, use naproxen or acetaminophen. Take a warm or cold shower and lie down with a cool cloth on your forehead. If you still have a headache, check with your doctor whether it is indeed a tension headache or a migraine. You may have jaw clenching or teeth grinding during your sleep. If your bite seems off, see a dentist. For stress control use relaxation techniques.
Other ways to treat tension headaches
Some suggestions sound mundane enough, but they can be effective: Get enough sleep, get enough exercise, and work on improving your posture. A physician trained in trigger point injections with local anesthetics (often anesthetists or general practitioners) can freeze your suboccipital and supraorbital nerves with lidocaine, which I have seen to work in 60% to 70% of cases in my former practice.
Conclusion
Pain treatment can be confusing as pain itself can be very multifaceted. The key is to search for the cause of the pain. Then treat pain very quickly. This way it has time within 2 to 3 months to turn into a chronic pain condition. Chronic pain is much more difficult to treat. The physician should treat acute pain successfully. Conventional medicine has to yet learn from naturopathic medicine and alternative medicine practitioners. They use prolotherapy, stem cell therapy, IMS and trigger point injections with local anesthetics. In addition low-dose laser therapy (Weber medical system) are valuable alternative methods to treat pain. These methods can successfully treat pain conditions. The physician can incorporate them into general medical practice.