In the first place I am discussing stem cell treatments that are currently available. By the same token stem cells got a bad reputation in the beginning of stem cell research. As a matter of fact, researchers at that time thought that embryonic stem cells were necessary to treat degenerative conditions. Be that s it may, immediately this raised an ethical flag, as physicians would harvest embryonic stem cells from a dying fetus. Similarly, this created a lot of unnecessary division among the public and scientists. To put it another way, it turns out that for most treatments there are enough stem cells in the body. As I will explain below, this was not general knowledge in the beginning.
Dolly, the sheep
With this in mind, the next bad rep came from Dolly, the sheep that was born on July 5, 1996. She only lived for 6 years, because the telomeres were short like that of an old animal and she died of a progressive lung disease. It is important to realize that researchers used a complicated stem cell technique to create Dolly. The method went under the name of “somatic cell nuclear transfer”. Three animals were necessary to achieve this. Researchers used an unfertilized egg from one animal from which they extracted the nucleus. The second animal donated a cell nucleus of a breast gland cell. A third animal served as a surrogate mother. After some cell divisions the researchers introduced the blastocyst into the uterus of the surrogate mother who carried baby Dolly until birth.
Mesenchymal stem cells and bone marrow stem cells
Fast forward to 2013. We now know that stem cells are fragile cells that do not like too much manipulation. Stem cells have long telomeres so they are younger than the typical cells of the body. Stem cells are present in the bone marrow, in fatty tissue and many other organs. In the last few years research has shown that this has already translated into practical applications. Originally researchers thought that stem cells were cells that could develop into any variety of body cell. Physicians at that time thought that stem cells would derive from bone marrow or from fetal tissue. Scientists called these cells “pluripotent cells”.
Induced pluripotent stem cells and mesenchymal stem cells
In the last years researchers could show that it was possible to turn off the SP100 gene could also prompt a body cell to become such a versatile, pluripotent stem cell. They are called “induced pluripotent stem cells” to distinguish them from embryonic stem cells, which have been highly contentious with religious groups. In recent years matters have been simplified with the observation that mesenchymal stem cells are distributed freely throughout the body and can be harvested fairly easily from fatty tissue by liposuction. Physicians prefer this latter technique, as it does not involve any manipulation of the stem cells themselves.
Here are a few examples of what is happening now and what developments are probable in the future:
Minimal invasive face-lift, called “space lift”
Mesenchymal stem cells are freely available in fatty tissue. Plastic surgeons in the US and elsewhere are using mesenchymal stem cells for a minimal invasive plastic surgery. In this “space lift” procedure the surgeon removes fat by liposuction. A cell separator separates the fat graft into a fat cell fraction and into a mesenchymal stem cell rich fraction. The physician injects fat cells and stem cell rich fraction together into various areas of the face where subcutaneous tissue is needed.
Facial rejuvenation
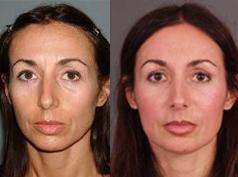
The mesenchymal stem cells enable the fat cells that were transplanted to latch on to the small vessels in the transplanted area so that they survive permanently. The result is a more youthful appearance of the face (see image). This is the secret of film stars in Hollywood. Nowadays the plastic surgeons in Beverly Hills do not do the conventional facelifts so much as they lead to artificially looking faces. They rather do the minimal invasion space lift for the natural look.
Knee problems, hip problems and lower back problems
Why wait with degenerative diseases of the knees, hip or of the lower back until there is permanent scarring and disabilities? Physicians can inject the mesenchymal stem cell rich fraction (without the fat cells this time) into diseased joints. This is a useful tool for degenerative changes in knee joints, hips and facet joints along the spine. The result is that the transferred mesenchymal stem cells recreate cartilage and the patient becomes pain free and regains mobility! But as with other diseases it is important to intervene early enough before permanent damage has set in.
Organ failures
Another exciting development is intravenous injection or injection via an arterial catheter into failing organs. Heart failure is an end-stage heart disease, where conventional medicine has nothing to offer other than symptomatic supportive medication. In contrast, physicians can inject mesenchymal stem cells into the blood. The pluripotent stem cells will find the weak areas in the heart muscle. It is there that they transform into heart cells and give the existing heart cells a boost.
The result is that the heart pumps more forcibly and the symptoms of heart failure disappear.
Parkinson’s disease and liver failure
Similarly, there are trials that show that Parkinson’s disease can be positively influenced with injections of the mesenchymal stem cell rich fraction.
Treatment of patients with liver failure using mesenchymal stem cells is being investigated, but is still in its infancy.
Chronic kidney failure
With regard to mesenchymal stem cell treatment of chronic kidney failure early human experiments on 30 patients showed very encouraging results.
Although this field is very promising, more caution is in order with regard to laboratory-manufactured stem cells. Researchers need to do more trials to show that they are ready for use in regenerative medicine. They have to show similar or even better successes as the present results achieved with mesenchymal stem cells. Physicians harvested mesenchymal stem cells directly and did not change them as described above.
More information on:
1. stem cells for stroke victims: http://nethealthbook.com/news/stem-cells-help-stroke-victims/
2. stem cells for knee osteoarthritis.






With havin so much content do you ever run
into any issues of plagorism or copyright violation?
My blog has a lot of exclusive content I’ve either created myself or outsourced but it looks like a lot of it is popping it up all over the internet without my authorization. Do you know any ways to help prevent content from being stolen? I’d certainly appreciate it.
I do not know how much plagiarism or copyright infringement is going on. For myself, I make sure I include links with reference to the original material I am referring to. I write all of the material myself. If you concentrate on fair publishing rules, you will not have any problems. I have been on the Internet since 2002. No problems. My hope is that at least some people learn something about how to stay healthier for longer…that’s the idea of anti-aging medicine.
Greetings from California! I’m bored to death at work so I decided to check out your site on my iphone during lunch break. I love the info you present here and can’t wait
to take a look when I get home. I’m surprised at how quick your blog loaded on my cell phone .. I’m
not even using WIFI, just 3G .. Anyways, great site!
I have been surfing online more than 4 hours today, yet I never found any interesting article like yours. It is pretty worth enough for me. In my view, if all web owners and bloggers made good content as you did, the web will be a lot more useful than ever before.
My relatives every time say that I am killing my
time here at net, but I know I am getting familiarity daily by reading such fastidious articles.
Print out a blog that you think is particularly important to take note for one of your relatives. See whether they still think it is ridiculous. They will want to know where you found this. Tell them that you did a Google or other search. Then show them where you found it. I promise you in time they will start searching on their own and stop ridiculing you…
You said this effectively!
wow! thanks for that tremendous report. I really cherished it . Hope you keep submitting this sort of amazing content articles
I have no intentions to stop them. Whatever I write will be factual, will be open-minded and yet be innovative in some way…