Recently I came across a book by Dr. Steven Masley, cardiologist (fellow of the American Heart Association, see Ref.1). The heart’s function is to pump your blood reliably all your life. It is a complicated organ, but it works well, if we treat it well. Western medicine has taught us that with complicated machinery and tests we can assess how the heart is doing. But until recently there was no reliable easier way to assess our cardiac health function. The purpose of this blog is to summarize a three-pronged approach to measure your heart and blood vessel health. It is described in detail in Ref.1, but I doubt that many people have yet read this important reference book. It is also important to FIRST see your doctor whether you are able to do the Bruce protocol (treadmill test, the third component below). If you neglect to be cleared by your doctor you run the risk of possibly getting angina pains or getting a heart attack.
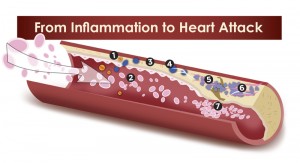
1. Carotid IMT or carotid intimal-medial thickness test: You measure the degree to which there is hardening of the coronary arteries indirectly by measuring the thickness of the lining of the carotid arteries (carotid IMT or carotid intimal-medial thickness test). Dr. Masley has showed over a period of 10 years and more in many patients at his Health Center that there is a close correlation between the degree of coronary artery hardening and the degree of hardening of the carotid arteries. He stated that his research has shown that “90% of the time, the carotid arteries, the coronary arteries, and even the arteries of your legs all grow plaque at the same time”. The gold standard for checking the condition of your coronary arteries is a heart catheterization as Dr. Masley explains (page 58). But he adds: “IMT testing should be the new gold standard for cardiovascular plaque testing. However, this is not yet the case. Despite its usefulness, 95% of doctors are not ordering this screening test for their patients. You can rest assured that this is a situation I am to change“.
2. A detailed lipid analysis called the VAP test: A detailed laboratory test analyzing your lipid fractions (LDL, HDL, total cholesterol and VAP test). The buoyant HDL fraction, called HDL2 is the key to having a low risk for hardening of the arteries. HDL2 is large, fluffy and is designed to remove garbage from within the lining of the arteries. Also, the cholesterol ratio is another measurement for a low risk for hardening of the arteries when it is less than 3.0. The first two tests assess how much hardening of the arteries there is present and when they are normal, there is a relative reassurance that nothing drastic (like a heart attack or stroke) should happen within the next 10 years provided you keep up a regular exercise program and healthy food intake.
3. Bruce protocol (Treadmill test): The Bruce protocol (treadmill test) is often done by a cardiologists, but can also be done through many gyms, where a trainer with experience in exercise physiology will do it. This functional test measuring cardiac output has been developed many decades back and has withstood the test of time. Here is an overview what this is. As the slope of a treadmill and the speed of the belt are increased, the heart needs to do more work to maintain blood flow to your extremities and vital organs. The trainer or exercise physiologist measures the response of the heart activity in relation to the increase of the exercise load. A complicated formula allows calculating how much your maximal cardiac output is. This test has several variations and can be complicated to understand. Essentially, the higher the numbers you can create, the better. Here is a table with various results of the VaO2max from Bruce protocols and how they are interpreted.
4. Treating abnormalities found with the three basic tests: These are the necessary tools that tell you where you are in regard to your heart function. People with heart failure should not do this third test, because their heart muscle is too weak to sustain this and they would get heart failure meaning that blood gets backed up into the lungs and there could be severe breathing problems leading to a lack of oxygen (anoxia) in the heart tissue, which in turn can cause irregular heart beats (fibrillation of the heart muscle) and a heart attack. Assume that the first two tests were within the normal limit for your age, then the Bruce protocol would give you the maximum heart output at the peak level of your treadmill test. At this point you are measuring directly the cardiac output (in other words what your heart is capable of pumping for you in a certain time unit). This measurement is what physicians call the VaO2 max or maximal oxygen consumption. This is the best index for maximal heart capacity. If your levels are higher than normal, you have extra reserves with respect to your heart as a pump for times when you need it. If this latter tolerance test shows poor results, it usually means that you were inactive and you would benefit from an exercise program. If the first test shows hardening of the arteries more than is appropriate for your age, you would need to look at your eating habits. At the same time often the VAT values and the cholesterol ratio is off meaning that you are eating the wrong foods and it shows in your blood test results.
5. Advise regarding diet, exercise and relaxation: Dr. Masley’s book has several sections that explain what needs to be done when things are not normal. For instance, the author does not mince words when it comes to eating the right fats and cutting out sugar and starchy foods. For instance on page 199 there is a neat table that lists the fiber content of different foods. We need more fiber to slow down the absorption of sugary substances, which will minimize the insulin response following a meal. Dr. Masley also mentions that omega-3-fatty acids from fish and good seafood choices will balance the omega-6-fatty acids that would lead towards the arachidonic acid pathway, which causes arthritis, inflammation and cancer. There are many more dietary recommendations, too numerous to repeat them all here. Suffice it to say that molecularly distilled omega-3 fish oil, vitamin D 1,500 to 3000 Units daily, and magnesium supplements are all good for you heart. Vitamin K2 gets calcium out of your blood vessels and into the bone (100 micrograms per day). Other worthwhile supplements mentioned in the book are CoQ-10 (50 to 200 mg twice per day), but it would be wise to have blood levels drawn, which should be above 2.5mcg/ml to which the CoQ-10 intake could be titrated. Curcumin and Resveratrol are also recommended. Most of all, it seems that regular physical exercise such as a balanced gym program is the single most effective way to reverse hardening of the arteries as measured by the carotid IMT testing.
Conclusion: Times have changed. It used to be thought that our lives were following a one-way street downwards. During periods of malnutrition, lack of exercise, being sessile and abusing alcohol and drugs this may well be the case. However, we now know that this is reversible. Change to healthier food, start smoothies with organic vegetables in a mixer, get going and walk. Jog or use a gym to get regular exercise. Physical exercise reverses the fat deposits inside the lining of the arteries. The HDL-2 fraction rises and helps counteract the elevated LDL cholesterol. Even the mood of the person who exercises regularly becomes more stabilized. Using these simpler three tests the physicians will not need the more complicated Thallium heart scans, heart catheterization etc. These three tests described above are well worth being done every two years, so that you can monitor what’s going on with your heart and blood vessels in general. What questions do you have? You could ask them below.
More information on heart disease: http://nethealthbook.com/cardiovascular-disease/heart-disease/
References: 1. Dr. Steven Masley, MD: “The 30-day Heart Tune-Up – A Breakthrough Medical Plan to Prevent and Reverse Heart Disease”, Center Street, A Division of Hachette Book Group Inc. New York, Boston, Nashville, USA © 2014.
Last edited Nov. 8, 2014