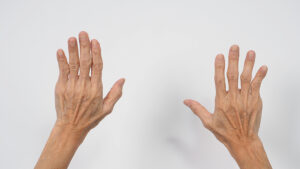
Researchers found that antibody treatment for rheumatoid arthritis was superior to conventional therapy. In particular, rheumatoid arthritis is an autoimmune disease where autoantibodies attack the synovial lining of joints. In this case, subsequently macrophages are activated, which attack joint surfaces. As an illustration, this process leads to crippling joint deformities.
The original study was published in June, 2019, but this is difficult to understand. The magazine Sciworthy published a review article on August 24, 2020 with more understandable language.
To emphasize, in mouse experiments the researchers found that only a small subfraction of activated macrophages caused symptoms of rheumatoid arthritis. They were folate receptor beta (FR-β) positive macrophages. It is important to realize that the researchers found them both in mice with rheumatoid arthritis and in man. The evidence in humans were the same findings in human tissue samples of people with autoimmune diseases.
Details of mouse experiments
Folate receptor beta (FR-β) positive macrophages are key in mouse model of RA
Explicitly, the researchers started experiments with a mouse model of rheumatoid arthritis, because it is easier to do than human research. They found that the key to developing rheumatoid arthritis was the presence of folate receptor beta (FR-β) positive macrophages. Chiefly, macrophages remove cell debris, bacteria or viruses from the blood. However, once they are activated and they carry FR-β receptors on their surface, they destroy joints. Certainly, in the mouse model monoclonal F3 antibodies were developed that kill activated macrophages. On the contrary, the human equivalent for the F3 antibodies is monoclonal antibodies with the name m909. They are directed at the FR-β receptors on the surface of activated macrophages. But first to the mouse experiments.
Inflammation from intraperitoneal injection of thioglycollate
In the first place, the researchers created an inflammatory condition by injecting thioglycollate into their peritoneal cavity. They could demonstrate that inflammation did occur. With this in mind they found macrophages in the peritoneal fluid. There were a lot of activated macrophages in it. Histological slides were analyzed with the help of F3 antibodies. In this case they visualized the activated macrophages. Subsequently the researchers treated mice with varying concentrations of monoclonal F3 antibodies. They found that the higher concentrations cured intraabdominal inflammation of the mice.
Researchers used monoclonal F3 antibodies to treat mouse model of RA
The researchers treated collagen-induced arthritis next in a number of experiments. Several concentrations of monoclonal F3 antibodies were given to these mice. Other experiments showed that monoclonal F3 antibodies specifically attacked only the activated macrophages and killed them. The killing of the activated macrophages in the mouse model of rheumatoid arthritis cured the arthritis. Fig. 5 shows this.
Mice treated with maximum concentrations of monoclonal F3 antibodies showed decrease in bone density
Next the researchers treated rheumatoid arthritis mice with maximum concentrations of monoclonal F3 antibodies to treat the arthritis. The swelling of their paws went down completely. CT scans of the bone in the paws showed decrease in bone density, while untreated controls showed significant loss of bone density. Monoclonal F3 antibodies were indeed a cure for RA in mice (Fig. 6).
Human experiments
Researchers confined human experiments to tissue samples from patients with various autoimmune diseases. Skin biopsies from patients with psoriasis, scleroderma, and sarcoidosis showed the distribution of FR-β-positive macrophages by special staining. This staining technique used human monoclonal antibodies (m909) against human FR-β receptors on activated macrophages. The publication depicts images that show abundant activity in all three autoimmune diseases (Fig. 1).
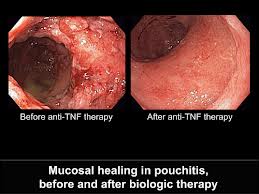
Researchers examined tissue samples from other autoimmune diseases with monoclonal antibodies (m909) against human FR-β receptors. The activated macrophages including rheumatoid arthritis, Crohn’s disease, ulcerative colitis and idiopathic pulmonary fibrosis lit up on fluorescence microscopy. In addition, nonspecific interstitial pneumonia, chronic obstructive pulmonary disease, systemic lupus erythematosus, psoriasis, and scleroderma tested positive as well.
Future therapy possibilities of rheumatoid arthritis with monoclonal antibodies
A series of experiments showed that two mechanisms can eliminate FR-β-positive macrophages: complement-dependent cytotoxicity and antibody-dependent cell cytotoxicity. It means that there is a strong possibility that autoimmune diseases may be treatable with monoclonal antibodies. Fig. 2 summarizes these experiments.
Conventional therapy for rheumatoid arthritis
To explain, the conventional treatment approach of rheumatoid arthritis is to induce a disease remission with drugs. To this effect doctors use anti-inflammatory drugs like ANSAIDs, disease modifying anti-rheumatic drugs (DMARDs). For example, drugs like methotrexate and sulfasalazine belong into this category. Unfortunately, the conventional drugs have many serious side effects that often make the rheumatoid arthritis patient’s condition worse.
In contrast, the integrative medicine approach to rheumatoid arthritis is to use dietary measures to reduce the inflammation. The fasting mimicking diet is able to reduce the severity of the inflammation in RA patients.
Other authors described the use of the Mediterranean diet to reduce inflammation. In addition, there are a number of regenerative methods that help improve the condition of RA patients. Research described here proved that antibody treatment for rheumatoid arthritis was superior to conventional therapy in a mouse model.
Discussion
Monoclonal antibodies (m909) against human FR-β receptors targeting activated macrophages opened up a new therapy method against rheumatoid arthritis. The equivalent F3 antibodies in mice were a useful tool to expedite research in this field. The publication that I reviewed here was able to combine mouse experiments and work on human tissue samples essentially showing the same results . Monoclonal antibodies (m909) against human FR-β receptors work potentially like a broad-spectrum anti-inflammatory drug. The monoclonal antibodies reduce the accumulation of inflammatory immune cells, which treats the cause of rheumatoid arthritis. This will likely be the future cure of rheumatoid arthritis and other autoimmune diseases. We urgently need clinical trials to prove in humans that the findings from a mouse model and human tissue samples are correct.
Conclusion
Researchers recently showed in a mouse model that a small portion of activated macrophages cause rheumatoid arthritis (RA). But they also examined many biopsies from patients with autoimmune diseases. The findings in human tissue samples were identical to the findings in a mouse model. Activated macrophages are sensitised to attack the linings of joints as is the case with rheumatoid arthritis. These macrophages develop special receptors, called folate receptor beta (FR-β), and the macrophages release cytokinins. The cytokinins (TNFα, IL-1, IL-6, IL-12 and others) cause inflammation and make the RA worse. They also recruit more neutral macrophages and convert them into activated macrophages. The research group found that monoclonal antibodies against human or mouse FR-β receptors killed the activated macrophages. This alleviated the arthritic symptoms and after enough antibody treatments cured the RA. There were no negative effects on the rest of the immune system.
Physicians will cure human autoimmune diseases with monoclonal antibodies in the future
Researchers demonstrated this mostly in a mouse model. But the authors have manufactured human monoclonal antibodies against the FR-β receptors of activated macrophages. This has set the stage for curing human autoimmune diseases with monoclonal antibodies as well. At this point there is a need for clinical trials with various autoimmune diseases including rheumatoid arthritis with monoclonal antibodies against activated macrophages.