Since its invention in 1978 there have been 5 million babies born through in vitro fertilization (IVF). According to the World Health Organization there are about 120 to 160 million couples worldwide struggling with infertility problems.
Assisted reproduction technology (a fancy name for artificial insemination) has been helped a lot by the breakthrough discovery in the US with regard to ultrasound identification of mature follicles in the ovaries. The second technical breakthrough, another ultrasound method done trans-vaginally to recover eggs from the identified mature follicles, has also helped the IVF technology (Ref.1).
When all of the cases of infertility in the United States are broken down into what causes them, the following was found (Ref. 2):
20% of cases of infertility were caused by anovulation, about 35% were due to abnormal semen production in the male, 30% by pelvic disease (fibroids, tubal blockage, polycystic ovaries), and 15% of cases were unexplained.
Process of artificial insemination
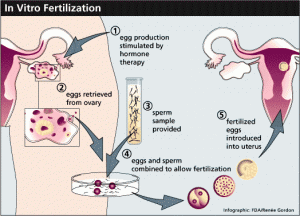
There are a number of steps that have to be followed to be successful with IVF.
a) Hormonal stimulation of the ovaries: The first step in getting eggs from a woman who desires IFV is to stimulate her ovaries to produce several mature follicles. This is achieved with gonadotropins, which are hormones that lead to ovarian overstimulation. Over the years this has been fine tuned with gonadotropin-releasing hormone (GnRH) analogues given first (stimulating release of LH and FSH from the pituitary gland). Subsequently follicle-stimulating hormone (FSH) is given, which causes the ovaries to produce follicles that can be identified on a TV screen using ultrasound technology. When follicle maturity is established with the ultrasound method, human chorionic gonadotropin can be given to trigger ovulation. However, when this is done and combined with artificial insemination through depositing sperm via a catheter into the uterus, the pregnancy rates judged by today’s standards to be too low (in the order of 15 to 20% per cycle).
b) Harvesting of eggs:
Nowadays the 2 or 3 follicles that have been identified as mature by ultrasound are used for follicular aspiration. With transvaginal sonography and a long needle that comes out from the ultrasound probe, the specialist will be able to harvest the mature eggs from the follicular cysts.
c) In vitro fertilization methods:
There are basically two methods for fertilization. First the standard IVF method is simply to add sperm to the eggs in a Petri dish with growth medium. After spontaneous fertilization the eggs undergo cell division. Compared to this standard IVF the success rates have been found to be higher with a newer method, called intracytoplasmic sperm injection (ICSI). In this case a single sperm is injected through a fine needle into the egg. On the 2nd or 3rd day of in vitro culture with either of these methods of fertilization the embryos consist of 6 to 8 cells. The embryos (typically one or two) are now introduced into the uterus of the mother by the specialist.
Success rates of in vitro fertilization (IVF)
Approximately 10% of all U.S. couples with women of the reproductive age are infertile, approximately more than 7 million women; the incidence of infertility steadily increases in women after the age of 30. Among fertile couples who have sex during the week before ovulation, about 20% achieve a pregnancy. If regular unprotected sex does not lead to a pregnancy within one year, the couple is considered infertile (that is the medical definition of infertility). With infertile couples using intrauterine insemination there is a pregnancy success rate of about 8 to 9% per cycle. However, IVF has a success rate of 30% per cycle. The chance of a pregnancy after six cycles of IVF is 72% provided the woman is in close contact with the IVF specialist and follows all of the instructions carefully. If the woman does not adhere to the program (this includes some dropouts), the pregnancy rate for IVF is only 51% in 6 months (Ref.2).
In 2010 the Nobel Prize for Physiology and Medicine went to Bob Edwards for his outstanding work on IVF. His work has improved the success rate for pregnancy of infertile couples significantly.
Costs of in vitro fertilization (IVF)
The conventional IVF cost is about 60,000$ to achieve a successful pregnancy; a newer, simplified IVF version costs only 265$, a method which has been developed for development countries. In the simplified version fertility drugs are given as generic tablets. The pregnancy rate for IVF is about 34% in this study from Belgium involving 100 infertile couples so far with the women being under the age of 36.
Gender selection and genetic abnormalities
Gender selection is highly controversial and is not being practiced. However, there are gender specific genetic abnormalities that can be identified in the 2 to 3 day old embryo after a few in vitro cell divisions. If DNA analysis shows an X-linked abnormality, this genetic abnormality would not be implanted into the womb. An embryo with a normal DNA test would be implanted instead (male or female). There are obvious ethical guidelines that have to be followed and these have been in place for a number of years.
The following overview of IVF contains a mini video showing a single sperm injection into an egg (the intracytoplasmic sperm injection method or ICSI). This is the latest in IVF technology, but also the most expensive option.
Complications with in vitro fertilization (IVF)
A review article in the Journal of Obstetrics and Gynecology in March of 2004 (Ref. 3) compared the complications and outcomes of single baby pregnancies (=singletons) that were either conceived normally (control group of 1.9 million spontaneous singletons) or conceived by IVF (12,283 IVF singletons pooled from 15 studies). Compared to normally conceived babies the group of IVF conceived babies had a perinatal mortality rate, which was 2.2-fold higher, the rate of preterm deliveries was 2.0-fold higher, low birth weight was 1.8-fold higher, a very low birth weight was 2.7-fold more common and the classification of “small for gestational age” based on birth weight was 1.6-fold higher. The medical researchers found a number of reasons for this: compared to normally conceived babies, the rate of IVF conceived babies had a higher rate of placenta previa, early preterm delivery, spontaneous preterm delivery, gestational diabetes, preeclampsia, and neonatal intensive care admissions were also significantly more common.
Other observations
If anovulatory cycles are the reason for infertility, clomiphene treatment can often restore regular menstrual cycles, but according to Ref. 2 there is an 8% risk for multiple gestations (twins, triplets) with a higher infant mortality rate.
For women with tubal obstruction IVF is better than attempting to do tubal reconstruction.
Women with unexplained infertility (no cause found despite thorough investigations) are treated by controlled ovarian stimulation as mentioned above and by inserting semen from the husband into the uterine cavity through a small plastic catheter (intrauterine insemination). With this combination pregnancy success rates of 10% per cycle can be achieved and this should be the first approach to cases of unexplained infertility (Ref.2)
Fibroids in the uterus are from estrogen dominance, so are polycystic ovaries. Replacement of missing progesterone with bioidentical progesterone cream will often shrink or melt the fibroids away, cure the ovaries of polycystic disease and restore fertility (this is not taught in medical schools and will not be told to most women attending fertility clinics). There are countless numbers of women attending fertility clinics needlessly; had they only checked their hormone status with saliva hormone tests and corrected the hormone imbalances with bioidentical hormones.
In vitro fertilization with or without ICSI has a pregnancy success rate of 50% per cycle for women less than 30 years of age. Above the age of 30 these numbers are lower and genetic abnormalities are higher necessitating the more expensive ICSI fertilization method. The pregnancy rate is also directly related to how many embryos are transferred into the womb. Usually 1 or 2 embryos are inserted. Twins are not uncommon with IVF.
Conclusion
In 35 years in vitro fertilization has developed into a sophisticated tool that helps women who previously were considered to be permanently infertile to conceive a normal pregnancy. Despite these technical advances we should not lose sight why infertility is such a problem today. Two main factors come to mind: sexually transmitted diseases can scar up the Fallopian tubes making it impossible for the sperm to reach their goal, the fertile egg. Men can also get scarring of their collecting ducts for the sperm (from epididymitis) from Chlamydia and other VD. Secondly, couples are settling into marriage much later in life, often well beyond their 30th birthday. Ideally a woman should have her first pregnancy between 20 and 25, when she is most fertile. If these things don’t fall into place, there is a cost to IVF and there are the associated risks discussed.
More information on infertility: http://nethealthbook.com/womens-health-gynecology-and-obstetrics/infertility-php/
References
1. Adam: Grainger & Allison’s Diagnostic Radiology, 5th ed. © 2008 Churchill Livingstone, CHAPTER 53 – Imaging in Obstetrics and Infertility.
2. Lentz: Comprehensive Gynecology, 6th ed. © 2012 Mosby: Treatment of the causes of infertility.
3. Review article in the Journal of Obstetrics and Gynecology in March of 2004 (March 2004, Volume 103, Issue 3: pages 551-563) examined the complication rates of IVF.
Last edited Nov. 7, 2014