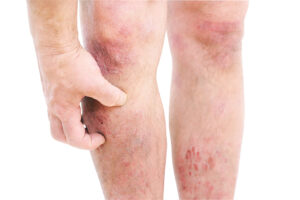
Notably, the use of biologics for treatment of autoimmune diseases is one of the newer achievements of medicine. In particular, a recent review summarized the use of biologics. For instance, chronic inflammatory conditions like skin eczema and asthma are some of the diseases where physicians use biologics.
Dupilumab (Dupixent)
It is important to realize that biologics are newer medications. They are mostly monoclonal antibodies developed in the lab and directed against various receptors. In particular, one of these is an interleukin-4 receptor. Specifically, this blocks inflammatory mediators such as interleukin-4 and interleukin-13. Dupilumab (Dupixent) is a monoclonal antibody. It must be remembered that it is a useful tool to treat atopic dermatitis (eczema), asthma and nasal polyps from chronic allergic rhinitis. For one thing, the common denominator for all these conditions is chronic inflammation. Here is more background information about Dupilumab. Specifically, this drug blocks certain proteins from attacking your own body. Besides, side effects of the drug are pink eye like inflammation of the eyes. Another side effect were mild skin rashes at the injection site.
Omalizumab (Xolair)
This drug is a monoclonal antibody also. It is given by injection into the skin every 2 to 4 weeks by a doctor or nurse. Originally it was developed for control of moderate to severe asthma. However, subsequently physicians treated moderate to severe atopic dermatitis cases also. Biologics are very expensive. It depends on your insurance carrier whether or not it is affordable for you.
Rheumatoid arthritis
Another disease that is autoimmune is rheumatoid arthritis. This can lead to crippling deformities in the hands and feet. Two of the earlier biologics for RA were etanercept (Enbrel) and adalimumab (Humira). But there are a host of other biologics that are effective as well. Generally speaking, the physician will start with conventional medicine, like Methotrexate. If Methotrexate does not sufficiently control the symptoms of rheumatoid arthritis, the physician usually adds biologics. Often patients need a combination of Methotrexate and biologics.
Different biologics affect different aspects of the autoimmune response. The first biologic for RA was a tumor necrosis factor (TNF)-antagonist, etanercept (Enbrel). Other TNF antagonists are infliximab (Remicade) and adalimumab (Humira). A different approach is an interleukin (IL)-1 inhibitor, called anakinra (Kineret). This biologic interrupts the inflammatory pathway of RA. Another biologic interrupts the T-cells or killer cells; it is called a T cell co-stimulation blocker, abatacept (Orencia). A different mechanism of action is the B-cell depleting agent, rituximab (Rituxan and Mabthera). This suppresses the formation of RA-autoantibodies from B cells.
The rheumatologist has a wide range of biologics from which to choose. The key is that the specialist individualizes the treatment protocol according to the response of each patient.
Crohn’s disease
Crohn’s disease and ulcerative colitis belong to the inflammatory bowel diseases (IBD). They are also autoimmune diseases where biologics can be useful.
There are three categories of treatment that are worth mentioning.
-
Anti-Tumor Necrosis Factor Agents
Adalimumab (Humira) was one of the first anti-tumor necrosis factor agents. The physician uses Humira in moderate to severe cases of Crohn’s disease and ulcerative colitis. It will calm down the symptoms of Crohn’s/ulcerative colitis and will maintain the disease in this symptom-free state. There are 8 other anti-tumor necrosis factor agents on the market.
-
Integrin Receptor Antagonists
These medications block a protein that coats the inflammatory cells. This arrests the cells, so they don’t move out into blood vessels and to tissues where they could cause tissue destruction. Examples are vedolizumab (Entyvio) and natalizumab (Tysabri). Unfortunately, natalizumab can have a serious side effect, a brain condition called progressive multifocal leukoencephalopathy (PML), This is caused by John Cunningham (JC) virus, which is a virus that 60% of the population carry. Natalizumab suppresses the immune system, which allows the JC virus to flare up and cause PML in the brain. Vedolizumab (Entyvio) is an alternative drug among the integrin receptor antagonists. Contrary to natalizumab it does not enter the brain. In a large clinical trial, it did not cause PML. This drug is infused over 30 minutes initially, then after 2 weeks, 6 weeks and every 8 weeks for maintenance.
-
Interleukin-12 and -23 Antagonist
Two inflammatory kinins, interleukin-12 and interleukin-23 are involved in causing inflammation in Crohn’s disease. They are proteins and the interleukin-12 and -23 antagonist helps to suppress the inflammation. The FDA approved ustekinumab (Stelara) for moderately or severe Crohn’s disease cases where conventional treatment did not show adequate responses. The physician administers the first treatment intravenously. The follow-up treatment occurs subcutaneously every 8 weeks by a nurse. Alternatively, the patient trains to self-inject the drug subcutaneously and administers the drug every 8 weeks.
Conclusion
Biologics have entered the treatment world of autoimmune diseases. Biologics can be monoclonal antibodies that inactivate part of an inflammatory cause, such as interleukins. Others may counter certain hyperactive immune cells. One of the side effects can be that the immune system is weakened. This allows latent viruses such as the John Cunningham (JC) virus to suddenly flare up. This is the case with progressive multifocal leukoencephalopathy (PML) following natalizumab (Tysabri) treatment for Crohn’s disease. Due to the development of new medications, this treatment is no longer the best option. Vedolizumab (Entyvio) is an alternative drug among the integrin receptor antagonists where PML does not develop.
Such varied conditions like rheumatoid arthritis, atopic dermatitis (eczema), Crohn’s disease and ulcerative colitis respond to biologics. In addition, nasal polyps from chronic allergic rhinitis and asthma also respond to these drugs. The physician has to carefully match the treatment option to the condition of the patient. The more specific the targets of biologics are the less immunosuppressive side effects they have.