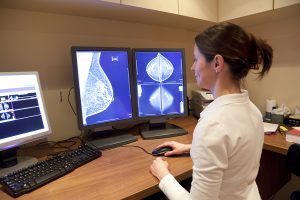
A new clinical trial suggests that less chemotherapy for breast cancer patients is necessary than what is the custom today.
70% of the common form of breast cancer, which is estrogen positive, but HER2 negative (more info below) has received treatment with surgery and subsequent chemotherapy. However, there was no scientific basis for this and this is what this large clinical trial was all about. The trial is discussed under this link. It has its origin in a medical research paper in the New England Journal of Medicine.
Estrogen positive, HER-2 negative breast cancer
The majority of breast cancers belong into this category. They have no signs of metastases and the Oncotype DX Breast Recurrence Score test has a score between 0 and 10. A woman with breast cancer like this does not need to undergo chemotherapy, because her long-term survival will not be any better on chemotherapy, and she can save all of the complications of chemotherapy.
The Oncotype DX Breast Recurrence Score
With this relatively new test 21 genes are tested in breast tissue from biopsies and surgical specimens. Dr. Otis Brawley, chief medical and scientific officer for the American Cancer Society, who was not part of the study explained: “What that test does is look at 21 different genes to see if each is turned on or off and then if it is over-expressed or not. So we have two yes-no answers for each gene. It looks at all 21 of those answers and gives that cancer a recurrent score between 0 and 100.” This number based on genetic cancer markers determines how likely the breast cancer is to reoccur in the next 10 years.
Relevance of genetic score test
A low score of between 0 and 10 on this test is indicative of good long-term survival. These patients will not need any chemotherapy. A medium score of 11 to 25 also has good survival as in this trial. However, scores of over 25 have an association with poor outcomes, when the patient receives only hormone therapy. In these cases the researchers say chemotherapy is also necessary in addition to hormone therapy.
Clinical trial regarding whether or not chemotherapy is necessary in the intermediate risk breast cancer patient
10,273 women were part of this trial between April 7, 2006, and October 6, 2010. 6,711 had test scores between 11 and 25, which placed them in the intermediate risk. Half of them received hormone therapy and chemotherapy. The other half received hormone therapy only. After an average of 9 years 83.3% of those on hormone therapy alone did not develop a recurrence of breast cancer. They also did not develop a second cancer. For the other group on both hormone and chemotherapy the rate was 84.3%. The difference between the two was not statistically significant. This established that the intermediate risk breast cancer patient does NOT require chemotherapy.
Results of clinical trial a surprise
This was a big surprise. Oncologists always included chemotherapy in the routine treatment schedule for these patients. But the trial clearly showed that hormone therapy alone was good enough! This allows thousands of breast cancer patients to avoid the devastating side effects of chemotherapy. Why would a woman undergo unnecessary chemotherapy, loose her hair, vomit and get stomach upsets? She may also suffer osteoporosis and undergo bone marrow suppression, which makes her more prone to serious infections.
Premenopausal women and those younger than 50
There is a group of women where breast cancer is more aggressive. Research followed this subgroup of women (premenopausal women and women below the age of 50) separately in the trial. More deaths occurred in the group that received hormone therapy alone. But death rates were much lower with a combination of hormone therapy and chemotherapy. If the score in these women was 16 or higher these women should receive the regular treatment consisting of surgery and hormonal measure). But they should also receive chemotherapy at the same time to reduce complications from their breast cancers. It has been known for many years that breast cancer in this particular patient group has a more aggressive growing habit. This trial showed that survival was a lot better in the group that did receive chemotherapy as well.
Surface markers of breast cancer
1. BRCA1 and BRCA 2
BRCA1 and BRCA 2 are rare mutations in some women who get early breast cancer, often on both breasts and often ovarian cancer as well. These are women who benefit from bilateral mastectomies, even when there is no cancer present yet.
2. HER2
HER2 is a protein that is expressed on the cell surface of some breast cancers. It leads to faster cell proliferation. Only about 30% of all breast cancers are HER2 positive. They respond to Herceptin and other medications listed in this link. In the past the prognosis for HER2 breast cancer was poor, now with better medication against this condition it has one of the more favorable outcomes.
3. ER and PR surface receptors
Estrogen receptor (ER) positive cancer cells will lead to faster tumor growth, when the patient receives estrogen. It also grows faster under the influence of estrogen or progesterone. About 65% of all breast cancers are hormone receptor positive (ER or PR). They will respond to drugs like Tamoxifen and others.(See this link)
Conclusion
Breast cancer diagnosis and treatment is rapidly changing. A clinical trial from the New England Journal of Medicine with over 10,000 women with breast cancer showed the following:
It is safe to treat women with an intermediate risk of breast cancer with surgery of the primary cancer and follow this up with hormone therapy. In the past these women were undergoing chemotherapy in addition, which has not shown better survival rates. On the other hand, premenopausal women or women below the age of 50 should receive treatment with chemotherapy to improve their long-term survival. Other factors to consider are the hormone receptors (ER and PR) and the HER2 marker. The Oncotype DX Breast Recurrence Score test has added a completely new dimension to breast cancer treatment as the New England Journal of Medicine article has shown. Overall breast cancer treatment has improved, which is good news for women.