A British study concluded that being a morning person can prevent depression. It was reviewed also in CNN. The study used sleep data from 85,000 UK participants in the Great Britain Biobank Study. They wore wrist activity monitors that provided sleep data. Researchers compared the sleep data with the self-reported mood changes. They found that if the sleep pattern is misaligned with the circadian rhythm, those who are night owls are at a higher risk of developing mood disorders. The controls were those who were morning persons. They were not affected by the misalignment effect.
Normal sleep pattern
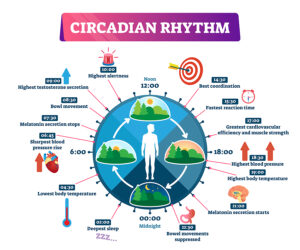
Natural sleep habit or the circadian rhythm starts between 10 PM and 11 PM and continues for 7 to 8 hours. Your hormones are replenished during your sleep. This helps your body’s hormones and the immune system to restore itself overnight.
“The health problems associated with being a night owl are likely a result of being a night owl living in a morning person’s world, which leads to disruption in their body’s circadian rhythms”. This is what sleep specialist Kristen Knutson said. She is an associate professor of neurology and preventive medicine at Northwestern University Feinberg School of Medicine.
Reclaim your natural sleep habit
The key is to learn to live within your circadian rhythm pattern. Caffeine is a powerful stimulant and will stop you from falling asleep. For this reason, it is best to avoid caffeine-containing beverages. If you cannot live without your favourite cup of java, switch to the decaffeinated version. Stop using LED lights (from TV, computers, tablets or smartphones) 2 hours prior to your bedtime. Use dark curtains and enjoy a comfortable bed. Maybe read that thriller, earlier in the day instead of making it your bedtime story. And do yourself a favour: you do not need the eleven o’clock news on TV! They will probably stop you from falling asleep. Go to sleep between 10PM and 11PM.
Children can have problems with sleep disturbances and depression
Another study published March 22, 2021 in the Jama Network showed that depression had an association with sleep disturbances in youth and children.
A meta-analysis of 16 publications looked at depression and disturbed sleep. It showed that depression was 1.5-fold higher in sleep disturbed youths/children compared to controls with a normal sleep pattern.
Other studies re. being a morning person can prevent depression
Another study with Dr. Knutson as the lead author appeared in 2018. The authors found that various health conditions, mood disorders and mortality were on the increase the more the sleep rhythm deviated from the circadian rhythm. Morning persons were protected from this effect. But night shift workers and night owls were at a higher risk of disease. Specifically, they found the following associations for evening types.
- Evening types compared to morning types had a 1.94-fold risk of psychological disorders
- The risk of diabetes was 1.30-fold for evening types
- Neurological disorders had a 1.25-fold risk in evening types
- Gastrointestinal/abdominal disorders occurred 1.23-fold more often in evening types
- respiratory disorders were 1.22-fold more common in evening types
- Evening types had a 10% increased risk of all-cause mortality
The researchers concluded that externally imposed timing of work and social activities has potentially serious health consequences.
Circadian misalignment responsible for disease
Dr. Knutson also said: “Circadian misalignment could also lead to inadequate sleep duration and quality, which could also impair mood and exacerbate mood disorders.”
In other words, circadian misalignment to circadian rhythm problems. This can cause mood disturbances, but eventually lead to the diseases listed above.
Evidence of health risks in night shifts workers
The medical literature is full of examples that the health of night shift workers is significantly affected by circadian misalignment. Here are a few examples.
1.Here is a random selection to illustrate the health risks of night shifts workers. A study from 2015 examined the sleep patterns of 315 shift nurses and health care workers in Iranian teaching hospitals. They found that 83.2% suffered from poor sleep and half of them had moderate to excessive sleepiness when they were awake.
2.This South Korean study examined 244 male workers, aged 20 to 39 in a manufacturing plant. Researchers compared blood tests from daytime workers to blood tests from night shift workers. They also obtained inflammatory markers like the C-reactive protein and leukocyte counts. Night shift workers had significantly higher values. The investigators concluded that shift workers have increased inflammatory markers. This is a sign of a higher risk of developing cardiovascular disease in the future.
Higher mortality and higher cancer risk in nighttime workers
3. A Swedish study found that white-collar shift workers had a 2.6-fold higher mortality over a control group of daytime white-collar workers.
4. Another study compared night workers in the age group of 45 to 54 with daytime workers and found a 1.47-fold higher mortality rate in the night shift workers.
5.In a study from China 25,377 participants were part of a study that investigated cancer risk in males with more than 20 years of night shift work. They had a 2.03-fold increased risk to develop cancer compared to males working day shifts. Women with night shift work in this study showed no effect with regard to cancer development.
Healthy telomeres with healthy sleep pattern
It is true that you can suffer multiple health problems, as all of your hormones depend on the resetting during your deepest sleep between 2AM and 4AM triggered by the nighttime melatonin response. Even your telomeres, the caps of chromosomes in every cell get shortened from too much stress and too little sleep.
One example of such a study comes from Milan, Italy. https://oem.bmj.com/content/75/Suppl_2/A480.1
In this 2018 study researchers compared 46 nurses who had worked in night shifts with 51 nurses working day shifts. Among the night shift workers breast cancer was common, but not among day workers.
Shortened telomeres, hypomethylation of BRC1 gene and p53 gene
In the night shift nurses from Milan there was hypomethylation of the breast cancer gene BRC1. There was also hypomethylation of the general cancer gene p53. At the same time significant telomere shortening occurred in night shift nurses who had worked night shifts for more than 15 years. This likely all worked together in causing night nurses to develop breast cancer more frequently.
Shortened telomeres mean a shortened life span. The reason for this is that people with shortened telomeres develop heart attacks, strokes and cancer. This is what shortens the life span. How do we avoid this risk? Go back to healthy sleep habits. As mentioned above it is best to start going to sleep between 10PM and 11PM and sleep for 7 to 8 hours. Night owls delay going to sleep by 2 to 3 hours.
Conclusion
A publication in Molecular Psychiatry demonstrated that evening person (night owls) are more likely to develop depression. This is in comparison to morning persons. As discussed, other researchers showed that evening persons also can develop diabetes and neurological disorders. In addition, respiratory disorders and gastrointestinal disorders are more common in night owls as well. When it comes to mortality, evening persons have a 10% increase of mortality over morning persons. There is a large body of literature regarding diseases of night shift workers. Night Shift work is perhaps the most extreme example of a circadian misalignment. It leads to poor sleep, inflammation in the body, increased cancer risk and higher mortality compared to day shift workers.
Prevent telomere shortening
Even the telomeres get shortened in night owls and night shift workers. We can prevent problems like these by going to bed in time and sleeping according to our circadian rhythm. If you had a poor night’s sleep, make up for it with the help of an afternoon nap. Do not sleep all afternoon though; half an hour or one hour will be enough. Even a short, restful nap after coming home from work can restore your feeling of wellness.