In the following I will describe 16 foods, which are the best foods for your heart. I will also comment as to why I believe they are best. This review is based on this article in “Medical News Today”.
But I have added many other comments to it.
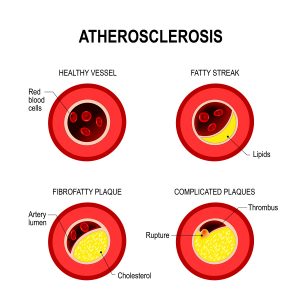
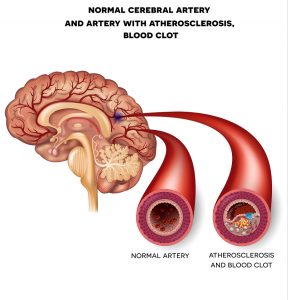
Heart disease is still the number 1 killer. We need to change what we eat.
Vegetables
The regular intake of green leaf vegetables and cruciferous vegetables (broccoli, cauliflower and cabbage) has an association with the preservation of cognitive function. In the Nurses’ Health Study starting in 1984 women were asked about their usual intake of a specified portion of food items, including 15 fruits and 28 vegetables. At a later date, between 1995 and 2001, researchers decided to ask the oldest participants (70 years and older) to participate in a cognitive function study. Two years later researchers repeated these tests.The main finding of the study is that women with the highest intake of green, leafy vegetables had the least decline in their cognitive function. The vegetable lovers, who consumed five serving of cruciferous vegetables, like broccoli, cabbage and cauliflower had less decline in their cognitive function. On the other hand the highest decline showed up in the group that averaged only 2 servings per week.
Asparagus
Asparagus is a source of fiber, folate, multiple vitamins and chromium. Chromium enhances the function of insulin to transport sugar into cells. Asparagus contains glutathione, a powerful antioxidant that neutralizes free radicals and carcinogens. It is said to help prevent lung cancers, larynx cancer, and bone, breast and colon cancers.
Berries
Berries like strawberries, raspberries, blackberries and blueberries are full of bioflavonoids. These are antioxidants, which prevent cardiovascular disease.
It is the anthocyanines, which prevent oxidation of LDL cholesterol. Berries also have bioflavonoids and reduce lipid formation in the blood. Berries contain fiber, folate, iron, calcium, vitamin A, and vitamin C.
Broccoli
This fiber rich vegetable helps to prevent hardening of the arteries. Broccoli and kale likely have preventative effects against colon cancer.
Chickpeas, beans, peas and lentils
Legumes or pulses are a great way to consume plant-derived protein. People who are on vegan diets should be eating them for a protein source. They also contain lots of fiber, vitamins and minerals. We know that they lower cholesterol, which prevents heart disease. Other healthy nutrients they contain are bioflavonoids, which have antioxidant properties and help prevent cardiovascular disease.
Dark chocolate
This is a food rich in antioxidants. Dark chocolate is chocolate with more than 70% cocoa content. Please note: “milk chocolate” is nothing better than candy and devoid of any health benefits. Dark chocolate increases the protective HDL cholesterol and prevents oxidation of LDL cholesterol. It is said to prevent atherosclerosis (hardening of the arteries). Don’t exceed eating 1 to 2 oz. per day, as chocolate has some sugar in it and the fat content would be detrimental with higher consumption.
Chia seeds and flaxseeds
Chia seeds and flaxseeds are rich in omega-3 fatty acids in the form of α-linolenic acid (ALA). ALA reduces LDL cholesterol and it dissolves plaque in the arteries. ALA also reduces blood pressure to a certain degree. All of this helps reduce cardiovascular disease (heart attacks and strokes). Note that flaxseeds must be ground to powder to release the nutrients from its tough shell. Both chia and flaxseeds can be used as an egg replacement in vegan cooking.
Fish high in omega-3s
Omega-3 fatty acids are abundantly present in fish. It has plaque-reducing properties and also reduces the risk for abnormal heart beats. Overall this means less cardiovascular disease. The American Heart Association recommends a 3.5 oz. serving of fatty fish (salmon, mackerel, lake trout, herring or sardines) twice per week.
Coffee
A Brazilian study from 2018 showed that drinking 3 cups of coffee a day would stop coronary artery calcification. Many other studies have shown reduced mortality from heart attacks and strokes with increased coffee intake.
Green tea
Green tea is known to reduce blood pressure slightly and to reduce cholesterol. Both effects are beneficial for the cardiovascular system (prevents heart attacks and strokes). Green tea also prevents many cancers. Whatever we know about coffee consumption seems to also be true for green tea consumption.
Nuts
Nuts contain healthy fatty acids (omega-3). But they also contain fiber, protein, minerals, vitamins and antioxidants. Use them in desserts, in salads and as a quick food on the go. They are definitely healthier than protein bars.
Liver
Liver is one of the nutrient rich foods. It is rich in iron, phosphorus, vitamin A, folate, vitamin B12 and biotin.
Oatmeal
Oatmeal is rich in soluble fiber. It has been shown to lower LDL cholesterol and total cholesterol. This is important for prevention of heart disease.
Red wine (may be)
The bioflavonoids of red grapes have been the subject of much research. There is a dose-response curve showing a protective effect with regard to heart attacks and strokes with the consumption of 1 to 3 glasses of red wine per day. But unfortunately there is also a dose-response curve with respect to alcohol consumption and cancer causation. Personally, I take resveratrol from the health food store, 500 mg daily and consume white wine or red wine very rarely.
Tomatoes
There are a number of beneficial phytochemicals in tomatoes. Carotenoids like lycopene, lutein, zeaxanthine and beta-carotenes are helping to prevent prostate cancer and colon cancer. Potassium and folate are cardioprotective.
Spinach
Eating spinach regularly will provide you with magnesium, iron and bioflavonoids. Magnesium is good for a regular heart rhythm. The other nutrients are good for skin, bone and hair health.
Discussion
I have reviewed why these 16 foods are the best foods for your heart. We have seen that many foods that are rich in antioxidants are also cancer preventative. People who eat a Mediterranean diet will get these 16 foods, because their meals are balanced with nutrients. But if you eat a hamburger or a pizza you will not get balanced nutrients. The more one-sided your food intake, the more dangerous your lifestyle becomes. This is the problem with the Standard American diet (“SAD”). You need all of the components of the 16 foods described here. Junk food won’t do, as it consists only of empty calories.
Conclusion
It is useful to review healthy foods as was done above. Now it is a matter of including them in your daily food intake. If this is overwhelming you, start with baby steps. One or two healthy foods here or there are a good start. Increase this until you cover all the 16 foods mentioned. The more balanced your food intake is, the more antioxidant vitamins you will get. And the more heart disease and cancer prevention you will experience.
Apart from good, balanced nutrition we also need regular exercise for heart disease and cancer prevention. Go to a gym, go for a walk, climb some stairs. Get away from the computer and television. Together with best foods for your heart this will keep you healthier for longer.